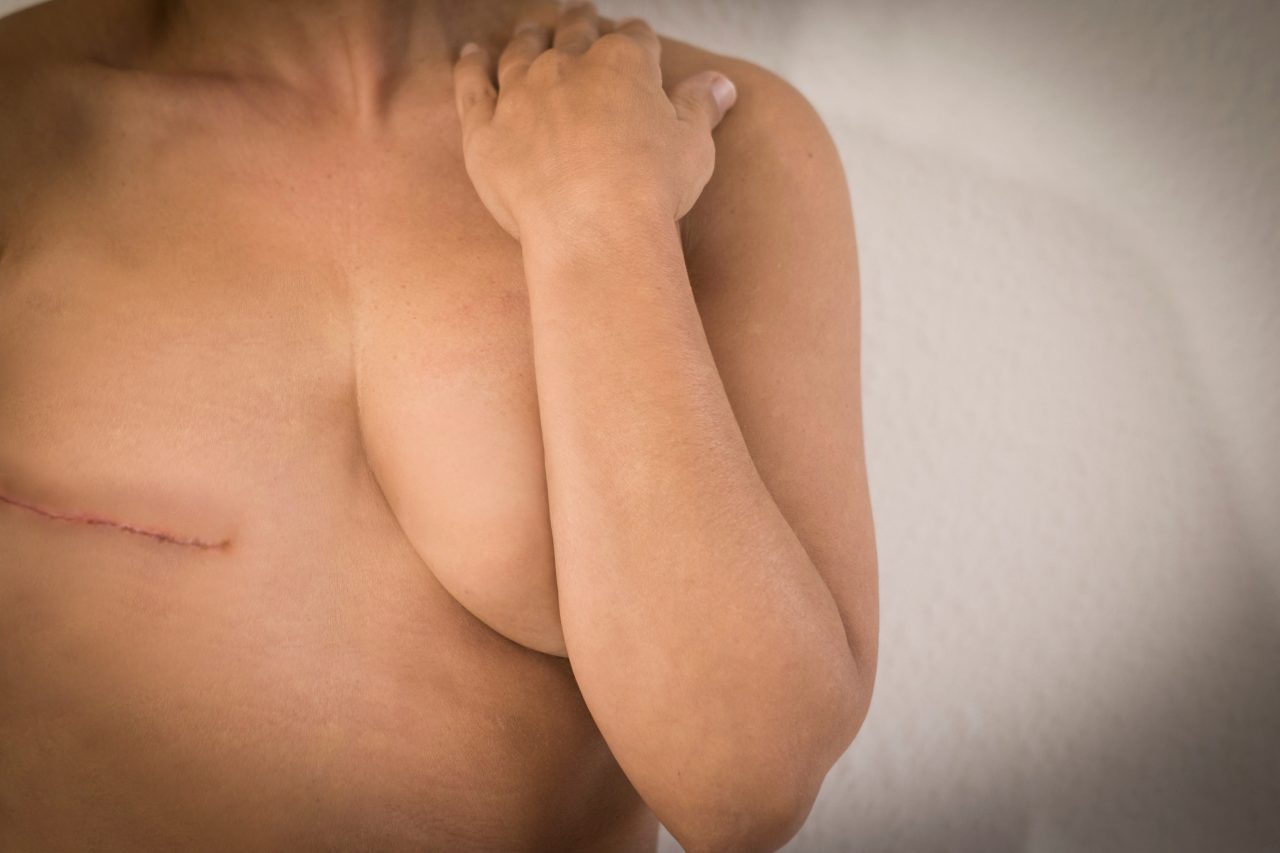
An Early Diagnosis of Cancer Leads to a Higher Chance of Treatment Success
In our new series, Best Advice from Women, for Women, Ms Jayde Simpson, an expatriate from the United Kingdom shares with us on finding out about her breast cancer diagnosis, coupled with the discovery of a high-risk gene.What kind of breast health issue did you face?I was diagnosed with Stage 2 Breast Cancer, which was ER+ PR- and HER2.How did you discover it?I felt a lump whilst on vacation that didn’t go away. Upon my return I scheduled an appointment with a breast specialist who performed an ultrasound. Within the week I had a mammogram, MRI and a PET scan which confirmed the suspicion. However, it wasn’t until a biopsy was conducted that it was confirmed as breast cancer.What was your biggest revelation after you were diagnosed?I did a gene test and discovered that I have a gene that makes my risk of breast cancer higher than the general population, although only a small number of cancers are hereditary. Lifestyle and other factors influence an individual’s risk profile.What is one thing you wish you knew before you started treatment?Understanding the type of breast cancer (ER/PR/HER2 positive or negative) can lead to different recommendations on the type of treatment you should get. I was upset when I had to get chemotherapy, believing what I had seen in the movies about the side effects from it. However, I sailed through this. A friend had recommended doing something nice around chemo and for me what stood out during my treatment was celebrating the end of each chemo with a lunch with a friend. My chemo duration had plenty of nice lunches and different friends supporting me throughout.What has the journey of dealing with or managing this issue been like for you?The absolute worst part was receiving the diagnosis as I did not truly believe this would happen to me and that all the tests would show this was a false alarm. The biopsy I received confirmed this was not the case. After that I did everything that I could to take a holistic integrative approach.I had a great breast surgeon and oncologist who partnered to give me the best medical treatment and tailored my treatment specific to me, e.g. my oncologist added a chemo that is shown to have more effect for people with the gene that I had, while my breast surgeon helped to add regular ultrasounds so we could measure the impact the chemo was having on reducing the tumour. This helped alleviate any anxiety on whether the treatment was working or not. I focused on ensuring that I did everything at home that I could to help – diet, exercise and I worked with a naturopath to identify supplements that would help me through the treatment.After the chemo I had a double mastectomy with immediate reconstruction and whilst this was a challenging decision, I did everything I could to minimise any future risk. I believe all of these things helped me to achieve a ‘pathological complete response’.The cancer diagnosis gave me the discipline I needed to prioritise me and ensure that I focused on a diet and exercise regime to best support my treatment. Despite the numerous rounds of chemo, I never once felt ill and felt stronger and fitter throughout. I had the odd tired day and some other limited symptoms. However, the treatment was nowhere near as bad as I expected.Before this cropped up, what was your attitude toward breast health?Sadly, I had a close friend who passed away from Breast Cancer and so I was very much aware of the need to do regular self-exams. The earlier you identify an issue, the more likely you have the chance of successfully dealing with it. I was aware of how my breasts would change during my regular cycle and so managed to self-identify the lump early enough to have a very successful outcome.Did this journey change that attitude?It only strengthened it. I am more in tune and aware of my body and if anything doesn’t feel right. I take care to watch stress levels and not overreact and am focused on ensuring that I have balance in my life with adequate sleep, exercise, supplements and focusing on what I eat (80% of the time).What do you think women in general feel about breast health?Whilst I was aware of the importance, I think I still thought of myself as being invincible and that something would not happen to me. I think women in general put other family members first and neglect to prioritise themselves. These two things together can mean that they neglect breast health. I also think sometimes people can feel embarrassed about seeking help or not wanting to expose themselves, or think “it’s probably nothing, I don’t want to bother anyone”.What are your thoughts when it comes to general awareness/education in this area?I hear of friends who tell me they don’t really know how to do a self-exam, or they skipped the last mammogram because they had to do something else and forgot to reschedule. I think they are missing the 2 most important factors here: 1. prevention is always better than cure (focusing on healthy lifestyle can reduce your risk) 2. the earlier you catch these things, the better your outcome. Whilst it’s rare, the tumour I had was not present on a mammogram but could be seen on the ultrasound, MRI and PET scan. My advice would be to listen to your body and if something doesn’t feel right, advocate for yourself and seek a referral to a breast specialist who can help allay any fears or help ensure you get treatment early.What advice would you give women about breast health?The risk is too high so early identification will give you more chance of success. Previously I did not prioritise myself, making excuses that I needed to attend to work, husband, children and that I had limited time. I now consider that prioritising my health means I will be around longer to enjoy time with my family. Ensuring I take steps to monitor my health and raising any concerns to my doctor means I’m around longer to enjoy my family. The earlier you detect something the more chance of success you have. Everyone I met throughout my journey was empathetic, caring, listened to me and addressed any concerns; the only downside is not acting early.