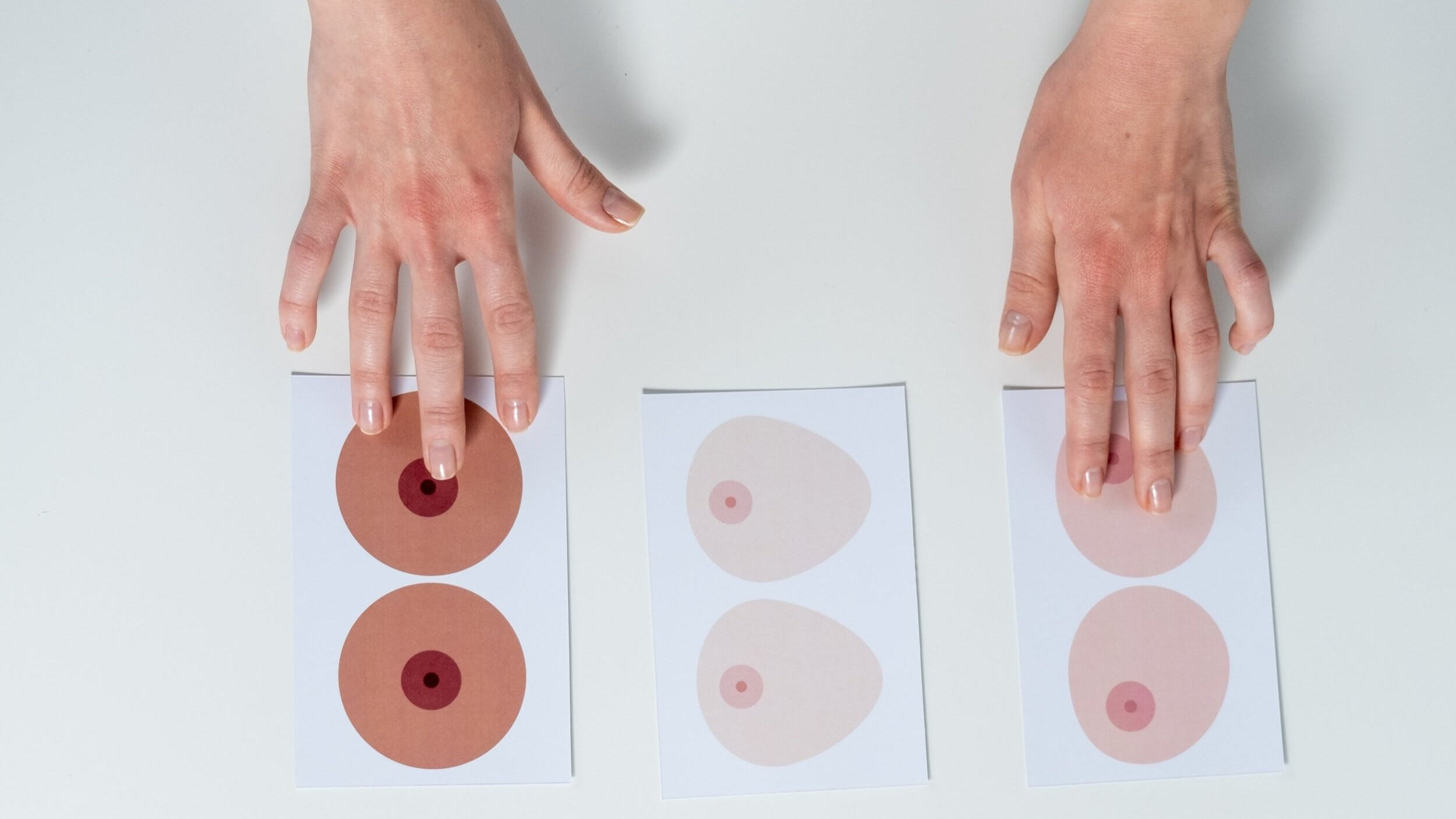
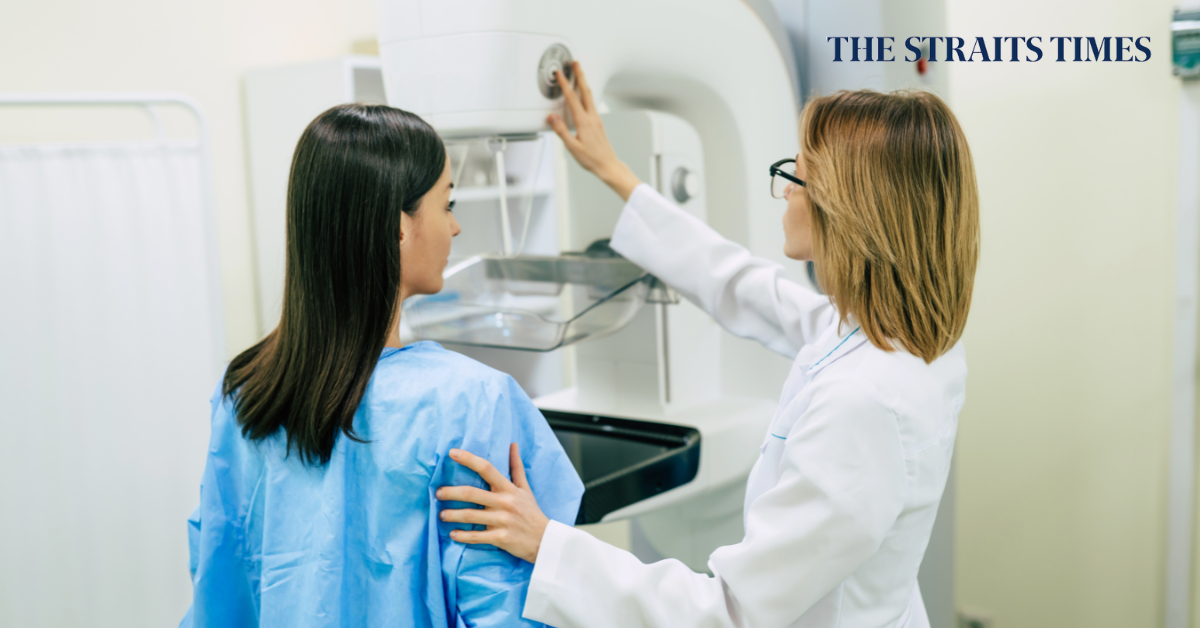
What Do Dense Breasts Have to Do with Breast Cancer?
Upon learning that breast density is linked to an increased risk of breast cancer, many women will be quick to check by touch or appearance if their breasts are dense. Unfortunately, breast density can only be confirmed with an imaging examination. Dr Lim Siew Kuan, our Senior Consultant and Breast Surgeon, shares more about some of the characteristics of dense breasts and how they relate to breast cancer.
What are the Characteristics of Dense Breasts?A breast contains varying amounts of fibrous, glandular and fatty tissue. To be considered dense, a breast should have less fat and more glandular and fibrous tissue than is expected.It is also worth noting that dense breasts are more commonly found in young women (premenopausal) as well as older women (postmenopausal) taking hormone therapy to address symptoms of menopause.The four main categories of breast density include:Category A: Breast is composed almost entirely of fatty tissueCategory B: Breast has scattered areas of fibroglandular densityCategory C: Breast has a mix of fibroglandular and fatty tissue, also known as heterogeneous densityCategory D: Breast has extremely dense tissue with little to no fatUnderstanding the Link Between Breast Density and Breast CancerTo this day, the reason for why dense breasts increase the risk of breast cancer is undetermined. However, certain metrics reveal why breast density is cause for concern.For some context: Oral contraceptives increase breast cancer risks for women 40 – 49 years old by 1.3 times. Heterogeneously dense breasts increase the risk by 1.2 times. Extremely dense breasts increase the risk by 2.1 times. And having a first-degree relative diagnosed with breast cancer before the age of 40 increases the risk by 3.0 times.Taken as a whole, breast density is a risk factor, but it is certainly not the biggest.A family history of breast cancer, a previous personal history of breast cancer or high-risk breast lesions, as well as hereditary mutations in the Breast Cancer (BRCA) genes are more important risk factors than breast density.Challenges in Mammogram DiagnosisDense breasts pose a significant challenge when looking for traces of cancer. On a mammogram, dense tissue is presented as a white area, but so too is breast cancer.The challenge for doctors exists in interpreting the mammogram, as cancer may be hidden under the guise of dense breast tissue.Nonetheless, mammograms are still the ideal choice for women with dense breasts; anecdotal evidence reveals that mammograms are more accurate than other diagnostic tests and can detect most types of breast cancer.Alternative DiagnosticsA combination of mammography and breast ultrasound is frequently used to increase the detection of breast cancer for women with dense breasts. The addition of ultrasound allows the visualisation of small breast lesions, which may be obscured by dense tissue on mammograms.Digital breast tomosynthesis (3D mammogram) is now widely available and is preferable to 2D mammography in screening women with dense breasts. It gives improved sensitivity for cancer detection, while decreasing the false-positive rates.Breast Magnetic Resonance Image (MRI) has also emerged as another excellent imaging modality, and may be used for further assessment when both mammography and ultrasound are non-conclusive. The benefit of using MRI is that, unlike mammograms, dense breast tissue does not affect imaging results. However, the downside is an increased likelihood of false positives.Due to its high sensitivity, MRI screening is also recommended in women with a high lifetime risk of developing breast cancer.RecommendationsIf tests conclude you have dense breasts, try not to worry too much, a discussion with a breast specialist will reveal what options are available to you based on your medical history and any other relevant factors.Yearly mammogram screening is advised, but for a more conclusive result, an ultrasound, breast MRI or even genetic testing may be recommended by your doctor.If you have discovered some signs and symptoms of concern, schedule an appointment with our breast specialists for medical advice on what are the best steps to take.Article contributed and reviewed by Dr Lim Siew Kuan, Senior Consultant and Breast Surgeon at Solis Breast Care and Surgery Centre.